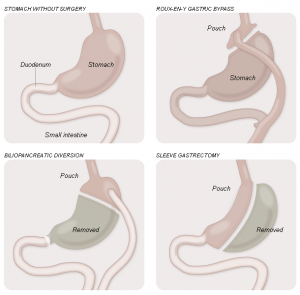
Courtesy of the NYTimes. This article today could not have been more timely as I’m slated to get the sleeve surgery shown in this diagram within the next few months.
Surgery for Diabetes May Be Better Than Standard Treatment
By DENISE GRADY
For some people with diabetes, surgery may be the best medicine.
Two studies have found that weight-loss operations worked much better than the standard therapies for Type 2 diabetes in obese and overweight people whose blood sugar was out of control. Those who had surgery, which stapled the stomach and rerouted the small intestine, were much more likely to have a complete remission of diabetes, or to need less medicine, than people who were given the typical regimen of drugs, diet and exercise.
The surgery also helped many to lower their blood pressure and cholesterol.
The new studies, published on Monday by The New England Journal of Medicine, are the first to rigorously compare medical treatment with these particular stomach and intestinal operations as ways to control diabetes. Doctors had been noticing for years that weight-loss operations, also called bariatric surgery, could sometimes get rid of Type 2 diabetes. But they had no hard data.
Experts say better treatments are desperately needed for the disease.
“Type 2 diabetes is one of the fastest growing epidemics in human history,” according to an editorial published with the two studies.
The question is whether major surgery, with its risks and complications, should be more widely used. Some surgeons and obesityexperts are pushing to establish a role for the surgeries in treating diabetes, not just obesity, while other experts say more research is needed.
The president for medicine and science for the American Diabetes Association, Dr. Vivian Fonseca, said the two studies were “not game changers” because they were relatively small.
The disease, which causes high blood sugar, is linked to obesity and often becomes harder to manage as it progresses. It can bring devastating complications like heart disease, strokes, blindness, amputations and kidney failure.
In the United States, the number of diabetes cases has tripled in the past 30 years to more than 20 million, according to the Centers for Disease Control and Prevention. Most of the cases are Type 2. Type 1, far less common, is not linked to obesity.
Researchers said the operations used in the studies help control diabetes not just because they make people lose weight — a known treatment for the disease — but because the changes in anatomy alter the levels of gut hormones that affect the metabolism of sugars and fats.
One of the studies, conducted at the Catholic University in Rome, compared two types of surgery with usual medical treatment. After two years, the surgical groups had complete remission rates of 75 percent and 95 percent; there were no remissions in patients who received medical treatment.
The second study, at the Cleveland Clinic, compared two types of surgery with an intensive medical regimen. The remission rates one year after surgery were lower than in the Italian study — 42 percent and 37 percent — at least in part because the American study used a stricter definition of remission. The intensive medical treatment led to remissions in 12 percent of patients.
Neither study involved the Lap Band, an implanted loop that cinches the stomach into a small pouch and that does not involve cutting the stomach or intestines.
The editorial accompanying the studies predicted that the new findings would have a major effect on diabetes treatment, and said that the operations “might well be considered earlier in the treatment of obese patients with Type 2 diabetes.”
But the editorial also noted that the studies were relatively small and did not go beyond two years. The writers said it was not clear whether the surgery would help diabetic patients who were not obese, or just not as heavy as those in the studies. The operations in the studies were performed by highly skilled surgeons, and results by others might not be as good.
Though the death rate from this type of surgery is less than 1 percent, patients nonetheless have died. There were no deaths in the two studies, but there were complications, including infection, nutritional deficiencies, bone loss and surgical problems that required repeat operations.
According to the American Society for Metabolic and Bariatric Surgery, about 200,000 bariatric operations are performed each year in the United States, and cost from $11,500 to $26,000. Some insurers cover them. Patients may lose 100 pounds or even more after the surgery. Most gain some weight back; some gain a lot back.
Guidelines from the National Institutes of Health say the surgery can be offered to people with a body mass index, or B.M.I. over 40, or over 35 if the person has diabetes or another illness related to obesity. The American Diabetes Association also says people with Type 2 and a B.M.I. over 35 should consider the surgery. Someone 5 feet 6 inches tall with a B.M.I. of 35 would weigh 215 pounds; B.M.I. of 40, 245 pounds.
Dr. Fonseca said the two studies would probably not lead the group to change its recommendations. He said the studies were small and short, and each was conducted at a single institution, so it was hard to know if the results could be replicated.
The study in Rome included 60 patients ages 30 to 60, with a B.M.I. of 35 or more. They were picked at random to receive medical therapy or one of two operations. The first operation, gastric bypass, shrinks the stomach into a small pouch and rearranges the digestive tract so that food enters the small intestine at a later point than usual. The second, biliopancreatic diversion, also shrinks the stomach. It alters the small intestine in a more extreme way.
The bypass patients had a 75 percent remission rate, and the biliopancreatic group, 95 percent. But the biliopancreatic group had more nutritional problems; the operation is usually reserved for people with extreme obesity and even then is not often performed in the United States
The improvements did not correlate with how heavy the patients were before surgery, how much weight they lost, their age, their sex or how long they had had diabetes. So it is hard to predict which patients will go into remission, said Dr. Francesco Rubino, who performed some of the surgeries in Rome and heads the Metabolic and Diabetes Surgery Center at NewYork-Presbyterian/Weill Cornell.
The Cleveland Clinic study included 150 patients ages 20 to 60, with B.M.I.’s from 27 to 43. Patients had intensive medical treatment, gastric bypass or sleeve gastrectomy, which cuts out part of the stomach, taking it from the size of a football to that of a banana. It is a somewhat simpler and safer operation than gastric bypass, and is growing in popularity. But the gastric bypass patients had a higher remission rate, 42 percent, than those with gastrectomy, 37 percent.
Dr. Philip Schauer, who led the study and performed the operations, said the remission rates were lower than expected. A possible reason was that the patients had very advanced diabetes.
For Heather Britton, 53, a computer programmer who lives in a suburb of Cleveland, the study was an opportunity. She was taking two diabetes drugs, but her blood sugar was out of control and so were her cholesterol, blood pressure and triglycerides. Diabetes runs in her family. Her mother died from complications of the disease.
“I wasn’t able to control it,” said Ms. Britton. “It was controlling me.”
She had the operation in January 2009. Within months, she was off medications for diabetes, cholesterol, blood pressure and triglycerides. By May, she had lost about 80 pounds. She gained some back, 13 or 14 pounds. But her health has been good.
“It’s been a total blessing,” she said.